3D-Printed Organs Nearing Clinical Trials
3D-Printed Organs Nearing Clinical Trials
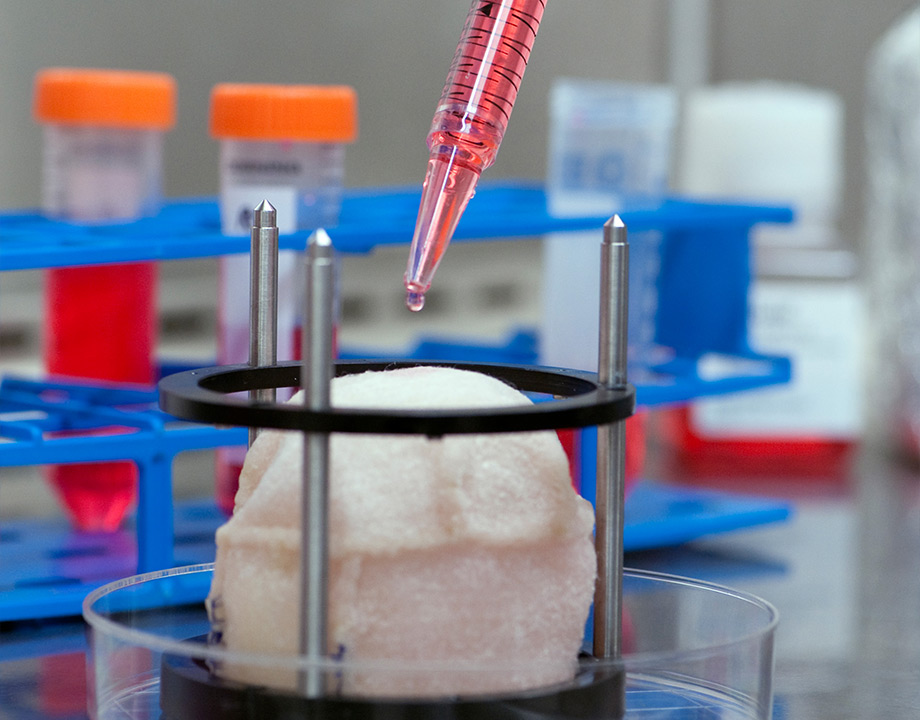

A 3D-printed matrix being seeded with bladder cells. While thick organs remain a challenge, artificial skin and blood vessels could be in clinical human trials within a year or two. Photo: Wake Forest
This story was updated on 1/18/2023.
With the aid of 3D printing and electrospinning, a team of bioengineers at the Wake Forest Institute for Regenerative Medicine, a research institute in North Carolina led by Anthony Atala, has been growing viable tissue and organs for patients. While many of these 3D-printed organs remain in the research stage, some should be ready for clinical testing within a year or two.
For more than 25 years, Atala has been working on generating tissue cells in the lab. From fingers and ears to kidneys and hearts, his team can now create 40 different organ and tissue structures.
What Is Electrospinning?
These procedures start by taking a small sample of the patient’s cells from the area bioengineers are trying to recreate—a skin graft about as large as a postage stamp, for example. Then, within a bioreactor, bioengineers replicate those cells until they’ve created enough to grow a new organ.
The next step is to build the extracellular matrix, or scaffold, on which the cells form. The team then seeds the matrix with growth promoters and biochemicals that prompt the cells to develop in specific ways. The matrix also provides mechanical forces that shape cell development.
To make structures such as skin or blood vessels, the lab uses electrospinning—a 3D printing technique that resembles the machines used to spin sugar into cotton candy.
Bioengineers use this technique to spin a hydrogel polymer at high speeds, forcing the polymer to elongate into long strands of fiber. They then place a thin rod in the center of the machine. The hydrogel fibers adhere to the rod just as fluffy cotton candy attaches to a paper cone. Scientists manipulate the shape of the spongey polymer by varying the voltage until they’ve mimicked the structure they are creating.
Further Reading: 3D Printing Living Skin with Blood Vessels
Once researchers achieve the desired shape, they spray cells from the bioreactor onto the matrix, layering it repetitively to match natural structures. To recreate skin, for example, they would start by applying cells from the subcutaneous layer and then those from the dermis and the epidermis.
Once layered onto the matrix, the structure is placed in an incubator that mimics the conditions of the human body. There, this combination of matrix, biochemicals, and cells begins to take on a life of its own using the matrix as a guide.
Although this technique is perfect for lightweight structures such as skin and blood vessels, it lacks the precision and ability to create solid three-dimensional structures—for example, a heart.
How to Print Solid Organs?
To create a solid organ, researchers need to promote the growth of blood vessels so that every cell in the organ receives oxygen and nutrients and can eliminate waste. Creating these blood vessel trees, which branch from large arteries into the tiniest vessels, has stumped researchers for decades. Yet Atala’s team has developed several potential solutions.
The first solution starts with an existing donor organ, such as a liver. First, bioengineers place it in a shaker (much like a washing machine) with mild detergents for about two weeks.
“After going through the shaker, you could hold the organ and it would look and feel like the organ, but it would have no cells,” Atala said. “Essentially, we’d preserved the skeleton of the organ.”
This skeleton is made of collagen, a protein found in the body’s connective tissue and its extracellular matrices. Like the electrospun matrix, the collagen matrix provides the structure and mechanical forces cells need to divide and take on organ-related functions. The organ skeleton is then deposited with the patient’s liver cells, which repopulate the organ, bringing it back to life with many of the functions of a human liver.
Although this method is promising, it still requires waiting for a donor organ. 3D printing may offer a way around that—it takes a lot more understanding of the organ itself, but promises to free patients from the waiting period.
Further Reading: 3D Bioprinter Prints Healthy Skin onto Patients in Minutes
“There’s so much going on in an organ like the heart that we can’t see unless we start from scratch,” Atala said. “We’re looking at the structure from a 360-degree perspective to make sure we can replicate the functionality of the organ in every way possible, or it won’t survive.”
One way to do that is to keep building organs and learn from the builds. To that end, Atala and his team have engineered over a dozen printers to carry out the complex processes of building a solid organ. The printers operate like color ink-jet printers—but instead of ink, their cartridges contain cells segregated by type.
To start, the bioprinter is loaded up with patient and organ information, which serves as a blueprint of what to build. Through a system of nozzles, the printer deposits layers of cells as a thick gel. This slowly generates the organ structure while preserving the life of the cells embedded within it.
While the team is still mastering this topographical form of engineering, 3D printing gives researchers a chance to work out the details. Through trial and error, they have been successfully programming the printers to deposit even the tiniest blood vessels within a complex organ.
Is 3D Bioprinting the Future of Organ Transplantation?
No matter which of these techniques the team uses, it takes about four to six weeks to build a healthy replacement for a patient. Because the replacement tissue or organ is made from the patient’s own cells, there is practically no likelihood of rejection—meaning patients heal quicker than ever before and don’t need to take medications to keep their immune system from attacking the transplant.
Further Reading: Top 10 Bioengineering Trends for 2020
“To be able to create these structures with a patient’s own cells to where they really can adapt and heal, that’s the hope for us,” Atala said. “We want to make sure that we can reach as many patients as we can.”
According to Atala, the more simplified structures like skin and blood vessels have already had successful human trials and will be in the clinic within a couple of years. Solid organs will take much longer.
It’s been a remarkable journey for Atala, and his advances have laid the foundation and knowledge base for successful human cell tissue generation.
Cassie Kelly is an engineering and environmental writer based in Columbus, Ohio.