Stanching Blood Flow with Microneedles
Stanching Blood Flow with Microneedles


A new bandage shows promise in slashing the number of deaths from blood loss.
The leading cause of death for people under 45 is the plain old accident. The sub-culprit of most of those accidents is excessive bleeding. The more quickly that bleeding can be stopped—on the battlefield, along the highway, or in the home—the more lives can be saved.
Now, researchers at the University of California, Los Angeles and Pennsylvania State University in State College have developed a new bandage that stops wounds from bleeding and begins clotting with remarkable speed.
The trick is a grid of microneedles. Such arrays of tiny prickers have already found application in drug delivery and cosmetic procedures for stimulating collagen production.
Become a Member: How to Join ASME
Reihaneh Haghniaz, a biotechnologist at UCLA’s Terasaki Institute for Biomedical Innovation, is lead author of the paper “Tissue adhesive hemostatic microneedle arrays for rapid hemorrhage treatment,” which appeared in the May 2023 issue of Bioactive Materials. She said she was “just curious if increasing the surface area and the contact area of the material with the clot can improve the hemostatic property or not.”
The bandage of microneedles that Haghniaz and her colleagues developed improved blood coagulation dramatically. Their microneedle arrays reduced clotting time from 11.5 minutes to 1.3 minutes.
Of course, the arrays needed some engineering before they were able to make such a massive difference to an injury. The researchers used silicate nanoplatelets, a material long known to help clotting, as part of their microneedles.
“Due to their specific structure, and also the surface charge that they have, they can attract platelets and improve blood coagulation,” said Haghniaz. The researchers also added a hydrogel, gelatin methacryloyl, to enhance the adhesiveness of the bandage.
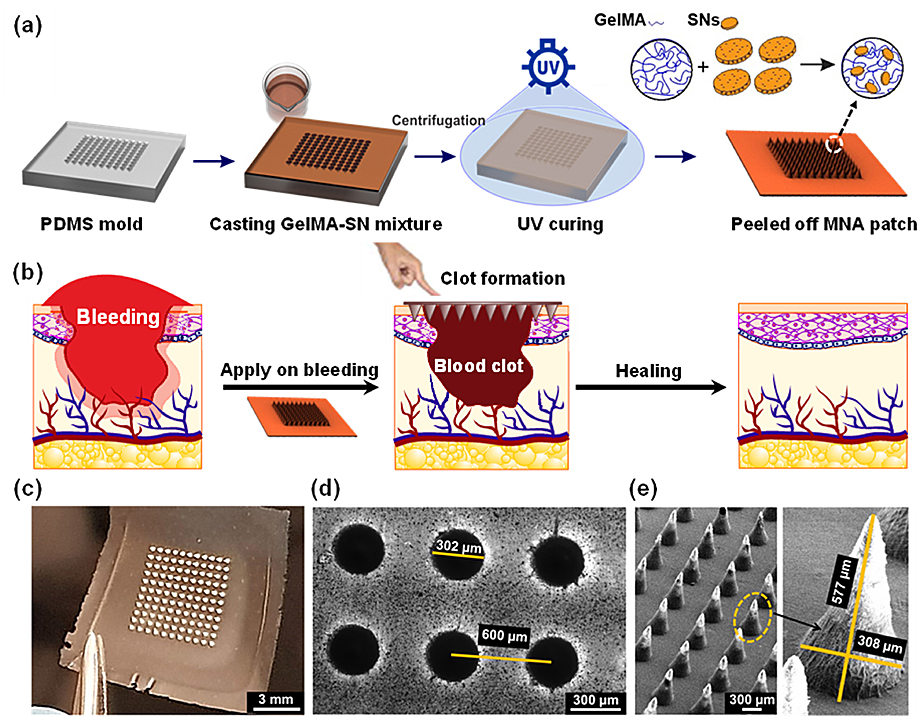
The microneedles themselves needed to be just the right length so that they would penetrate skin and adhere to the wound, but not go so deep as to harm blood vessels. Longer needles can break as well. The team settled on needles with a base diameter of 300 micrometers and a length of about 600 micrometers.
They tested their prototype, an 11 by 11 grid of needles, on four-millimeter lesions on rat livers, where they observed their coagulatory success.
The surface of a liver doesn’t present much of a challenge to sharp things of any size. To prove the penetrative qualities of their needles, Haghniaz and her team also applied them, successfully, to pig skin.
“The pig skin is much thicker and contains more fat that is more difficult to puncture,” she said. “So basically, they can puncture easily into human skin.”
More for You: Spinning a Bandage
The microneedle array itself does not induce any suffering or pain when applied. “They are definitely painless,” said Haghniaz. “The length of the needle is very little, really.”
The bandage is a such a straightforward and agony-free piece of technology that its application requires no medical expertise. The microneedles come inside an applicator, which, when pressed on, applies just the right amount of force onto the wounded area. Soldiers, EMTs, and parents alike can apply the bandage the moment it’s needed, with ease.
There is still development needed before the needle-based bandage finds its way into first aid kits. For now, the tiny array is only big enough for millimeter sized wounds. Scaling up is not expected to be difficult. But the researchers also hope to try different geometries, sizes, and densities of needles. They also plan to test their bandage for possible side effects and longer-term issues.
“We need to do more biological studies, specifically for inflammatory responses and scar formation,” Haghniaz said.
Michael Abrams is a technology and engineering writer in Westfield, N.J.
Now, researchers at the University of California, Los Angeles and Pennsylvania State University in State College have developed a new bandage that stops wounds from bleeding and begins clotting with remarkable speed.
The trick is a grid of microneedles. Such arrays of tiny prickers have already found application in drug delivery and cosmetic procedures for stimulating collagen production.
Become a Member: How to Join ASME
Reihaneh Haghniaz, a biotechnologist at UCLA’s Terasaki Institute for Biomedical Innovation, is lead author of the paper “Tissue adhesive hemostatic microneedle arrays for rapid hemorrhage treatment,” which appeared in the May 2023 issue of Bioactive Materials. She said she was “just curious if increasing the surface area and the contact area of the material with the clot can improve the hemostatic property or not.”
The bandage of microneedles that Haghniaz and her colleagues developed improved blood coagulation dramatically. Their microneedle arrays reduced clotting time from 11.5 minutes to 1.3 minutes.
Of course, the arrays needed some engineering before they were able to make such a massive difference to an injury. The researchers used silicate nanoplatelets, a material long known to help clotting, as part of their microneedles.
“Due to their specific structure, and also the surface charge that they have, they can attract platelets and improve blood coagulation,” said Haghniaz. The researchers also added a hydrogel, gelatin methacryloyl, to enhance the adhesiveness of the bandage.
The microneedles themselves needed to be just the right length so that they would penetrate skin and adhere to the wound, but not go so deep as to harm blood vessels. Longer needles can break as well. The team settled on needles with a base diameter of 300 micrometers and a length of about 600 micrometers.
They tested their prototype, an 11 by 11 grid of needles, on four-millimeter lesions on rat livers, where they observed their coagulatory success.
The surface of a liver doesn’t present much of a challenge to sharp things of any size. To prove the penetrative qualities of their needles, Haghniaz and her team also applied them, successfully, to pig skin.
“The pig skin is much thicker and contains more fat that is more difficult to puncture,” she said. “So basically, they can puncture easily into human skin.”
More for You: Spinning a Bandage
The microneedle array itself does not induce any suffering or pain when applied. “They are definitely painless,” said Haghniaz. “The length of the needle is very little, really.”
The bandage is a such a straightforward and agony-free piece of technology that its application requires no medical expertise. The microneedles come inside an applicator, which, when pressed on, applies just the right amount of force onto the wounded area. Soldiers, EMTs, and parents alike can apply the bandage the moment it’s needed, with ease.
There is still development needed before the needle-based bandage finds its way into first aid kits. For now, the tiny array is only big enough for millimeter sized wounds. Scaling up is not expected to be difficult. But the researchers also hope to try different geometries, sizes, and densities of needles. They also plan to test their bandage for possible side effects and longer-term issues.
“We need to do more biological studies, specifically for inflammatory responses and scar formation,” Haghniaz said.
Michael Abrams is a technology and engineering writer in Westfield, N.J.